By: Ranier Simons, ADAP Blog Guest Contributor
In the fight to eradicate HIV in the United States, testing is a fundamental and indispensable tool. Testing is the gateway to treatment and prevention. It is the only way to identify those who are HIV-positive, not only to get them into timely, appropriate care and treatment but also prevent transmission to others with Undetectable equals Untransmissible (“U=U”). Unfortunately, about 13% of people in the United States living with HIV/AIDS (PLWHA) are unaware of their status.[1] Whereas HIV self-testing has helped to overcome this barrier, it hasn’t been without its own challenges.
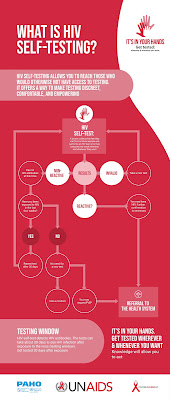 |
| Photo Source: PAHO |
Many people do not test for a myriad of reasons. Some do not have access to testing facilities due to transportation issues or lack of availability in their area. Stigma and fear hinder others. Presently, some still fear being seen in a testing clinic by people in their community, while others fear receiving a positive result. Cost is a barrier to those who lack healthcare insurance and do not have access to free clinics. To increase HIV testing, medical science has developed exceptionally effective HIV self-testing. It has been an invaluable tool.
HIV-self testing, in the past, required painful finger pricking to draw blood. Now, there are oral self-testing kits, such as OraQuick, that only require swabbing of the mouth and gums. Self-testing kits are much more affordable than going into doctor's offices for bloodwork. They also allow people to test in the privacy of their own homes and ensure their confidentiality. Moreover, some organizations provide free testing kits for those who can’t afford to purchase the over-the-counter ones.
As beneficial as HIV self-testing kits are in attempting to normalize testing, especially in high-risk groups, there are downsides. Testing in private means that there are people who will be alone when they receive a positive result. Self-tests, such as OraQuick, provide a 24-hour hotline for people to use for support and guidance concerning a positive or negative result. However, for some, that is not enough. A positive result's psychological gravity could be too overwhelming for someone to handle alone speaking with a support person over the phone. Studies have shown that PLWHA are 100 times more likely to commit suicide than the general population.[2,3] In a clinical setting, trained support professionals are available to help navigate a positive diagnosis. Moreover, a support hotline number is not guaranteed to be utilized. There’s the risk that people will deal with the diagnosis in a vacuum.
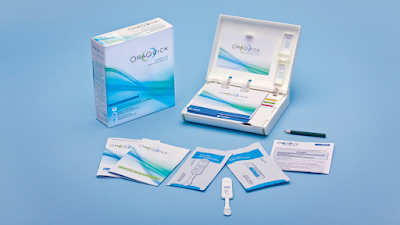 |
| Photo Source: U.S. Food & Drug Administration |
Self-testing also does not always result in people seeking treatment. Doctors recommend people confirm a positive self-test with clinical bloodwork. This is to verify the result and facilitate the swift initiation of an antiviral medication regimen. Studies show that some people do not seek out and initiate HIV treatment after a positive test result.[4] This can result in poor health outcomes from progression into later stages of HIV disease. Additionally, lack of treatment can result in additional virus transmission to others.
Self-testing also has potential adverse effects on those testing negative. Research shows that self-testing does not facilitate behavior modification in those who test negative. For example, data indicates that self-testing increases incidences of condomless anal sex among men who have sex with men (MSM).[4] Receiving a negative test result in a clinical setting provides the opportunity for discussion on ways to stay negative. This can include behavior modification as well as initiation of PrEP.
HIV self-testing reduces linkage to care by about 17%.[5] The lack of linkages to care not only impacts patients and their own healthcare, but also the community at large. In the U=U era of fighting the HIV epidemic, linkages to care are of paramount importance.
Therefore, it needs to remain a part of wide-ranging prevention efforts and needs targeted additional support. Self-tests can result in more people being tested; however, uncovering the population of unknown positive individuals cannot be the sole focus. Stimulating additional positive outcomes from self-testing will require innovation to bolster support.
[1] U.S. Department of Health and Human Services. (2023, October 3). U.S. Statistics. Retrieved from https://www.hiv.gov/hiv-basics/overview/data-and-trends/statistics/
[2] Wilder, T. (2021, October 8). The suicide rate for people with HIV is 100 times higher than the general population. The need for mental health care is urgent. Retrieved from https://www.thebodypro.com/article/suicide-rate-people-with-hiv-100-times-higher-than-general-population
[3] Cairns, G. (2021, August 11). The hardest outcome of all: HIV and suicide. Retrieved from https://www.aidsmap.com/news/aug-2021/hardest-outcome-all-hiv-and-suicide
[4] Adeagbo, O., Badru, O., Lucho, E. (2023, October 2). HIV self-test kits are meant to empower those at risk − but they don’t necessarily lead to starting HIV treatment or prevention. Retrieved from https://theconversation.com/hiv-self-test-kits-are-meant-to-empower-those-at-risk-but-they-dont-necessarily-lead-to-starting-hiv-treatment-or-prevention-213726
[5] Witzel, T. C., Eshun-Wilson, I., Jamil, M. S., Tilouche, N., Figueroa, C., Johnson, C. C., Reid, D., Baggaley, R., Siegfried, N., Burns, F. M., Rodger, A. J., & Weatherburn, P. (2020). Comparing the effects of HIV self-testing to standard HIV testing for key populations: a systematic review and meta-analysis. BMC medicine, 18(1), 381. https://doi.org/10.1186/s12916-020-01835-z
Disclaimer: Guest blogs do not necessarily reflect the views of the ADAP Advocacy Association, but rather they provide a neutral platform whereby the author serves to promote open, honest discussion about public health-related issues and updates.

No comments:
Post a Comment