By: Carine Carmy, Head of Marketing, Amino
When you need to find a doctor, how do you find the right one? If you have health insurance, you might start with your insurance plan, and check which doctors are in-network. You might look at online resources, and Google which doctors are located nearby. You might look at Yelp or other review sites to see what people say about the doctors (and if you’re lucky, those reviews might be relevant to your condition or to the procedure you need). If you have a friend or family member with your condition, or know someone with a medical background, you might be able to ask one of them for a recommendation.
Even if you went through all that to find a doctor, would you feel confident that you made the right choice? With all the resources available for health care decision-making, you might still be missing a crucial piece of information: how much experience does this doctor have with what you need?
Research shows that when it comes to doctors, experience matters—not necessarily years of experience practicing medicine, but rather the volume of patients a doctor has treated with your condition. That’s the philosophy behind
Amino, a free website that launched in October 2015, which lets you find and book doctors and estimate health care costs for medical procedures. With Amino, you can get matched with a doctor based on his or her experience with the condition you have or the treatment you need. Amino measures a doctor’s experience by analyzing data from health insurance claims (the records doctors send to insurance companies to get paid for what they do) to uncover what they focus on and how they treat their patients.
Below, you can use the embeddable Amino search to see how the product works and find doctors who have experience with HIV-related care and treatment—you can also change any of the search filters to look up other conditions or procedures (Amino has over 800 topics to choose from).
Here are five quick guidelines for using Amino:
1. If you’re looking for doctors who have experience with HIV-related care and treatment, you would first enter in some information about yourself or the patient you’re taking care of.
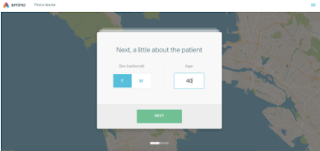 |
| Photo Source: Amino |
2. Then, enter your location and insurance (if you have it—it’s optional to enter in your insurance).
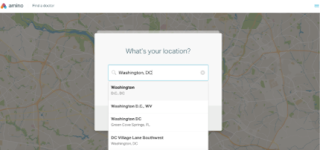 |
| Photo Source: Amino |
3. You’ll get a list of doctors who have the most experience with testing people like you—of the same age and sex, and with the same insurance—for HIV-infection. Amino will search its database of 893,000 doctors to provide this list. You might see a variety of doctors in your match list, and depending on your preferences you can filter by a doctor's specialty.
 |
| Photo Source: Amino |
4. When you click on the doctor’s profile, you can see what they treat patients for and which services, tests, and procedures they provide, along with other important information like their credentials.
 |
| Photo Source: Amino |
5. From there, you can book an appointment via email or text message at no cost to you.
Amino also offers cost estimates for 49 medical services and procedures for dermatology, diagnostics, men’s health, orthopedics, preventative care, surgeries, and women’s health—and you can view those cost estimates for individual doctors as well as research costs in your area and insurance network.
Health care is not one-size-fits-all—what’s right for you can change depending on your health and your preferences. Your search for a doctor should be customized to your condition or the procedure you need, and you should be able to see as much information about a doctor as possible before making the time commitment to see them in-person.
Using Amino, you get a data-driven and personalized experience, which can help you choose care with confidence. If you have any feedback or questions, please don’t hesitate to reach out to the team at
feedback@amino.com.
________
Disclaimer: Guest blogs do not necessarily reflect the views of the ADAP Advocacy Association, but rather they provide a neutral platform whereby the author serves to promote open, honest discussion about public health-related issues and updates.







