By: Ranier Simons, ADAP Blog Guest Contributor
As the current Monkeypox outbreak continues to develop, so does ongoing research and discourse. A previous blog post, HIV & Monkeypox: What Patients Need to Know,[1] discussed early research regarding possible connections between HIV and Monkeypox. One main takeaway was that clinicians need to expand the list of symptoms they look for in Monkeypox infections. The current outbreak is not behaving as it has historically in the areas of Africa where it is endemic. Symptoms and related conditions can be mistaken for other sexually transmitted infections (STI's) or other illnesses. Additionally, it was noted that clinicians should adopt a heightened caution and suspicion of Monkeypox disease in at-risk groups. Recent research strongly reinforces the need for clinicians to increase their efforts to look for monkeypox disease in at-risk populations and the need for targeted education and messaging.
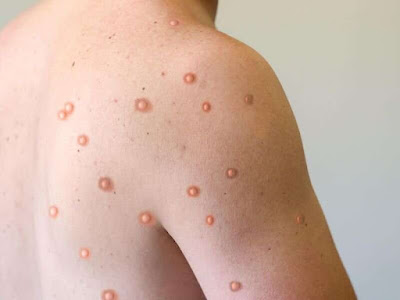 |
| Photo Source: Medical Express |
A report published September 9, 2022, in the U.S. Center for Disease Control & Prevention's (CDC) Morbidity and Mortality Weekly Report (MMWR) shows that people who are HIV-positive or have STI’s are disproportionately represented among those infected with Monkeypox.[2] Data from health departments in eight different U.S. jurisdictions was analyzed to examine Monkeypox clinical differences regarding HIV and STI status. Out of the 1,969 people infected with Monkeypox, who were 18 years of age or older, 38% (755) were HIV-positive, 41% (816) had another STI diagnosed in the previous year, and 18% (363) had both.[2] Additionally, those people living with HIV and also infected with Monkeypox had a higher prevalence of having an STI diagnosis in the preceding year than those diagnosed with Monkeypox who were HIV-negative.
A similar study published September 4, 2022, in HIV Medicine with a much smaller cohort was conducted in Germany.[3] In this study, 546 monkeypox infections from 42 sites were analyzed. All of the subjects were men who have sex with men (MSM). There were 256 (46.9%) patients living with HIV, mostly with viral suppression, 232 (42.5%) were taking pre-exposure prophylaxis (PrEP), and 58 (10.6%) had no HIV infection or PrEP use.
The likelihood of hospitalization of HIV-positive patients diagnosed with Monkeypox is still unclear. The CDC study indicates that co-infection with HIV may increase the risk of hospitalization but, the German study does not.[4] The CDC study confirmed hospitalization records from around 1,300 out of the 1,969 subjects. Eight percent of those hospitalized were HIV-positive and 3% were not. Conversely, the German study did not show a significant difference in hospitalization rates. Among those 546 men the overall hospitalization rates were 4% regardless of HIV status.
Both studies have limitations thus, cannot be used to provide definitive generalizations regarding clinical differences in Monkeypox infections between MSM with or without HIV. However, what is abundantly clear is the increased prevalence of the Monkeypox infections amidst MSM living with HIV, with STI’s or both. Evidence shows the heightened prevalence of HIV in populations that regularly receive HIV and STI health services. Thus, it is imperative that clinicians increasingly offer Monkeypox testing to those being treated for HIV and other STI’s in addition to increasing HIV and STI testing for those being treated for monkeypox.
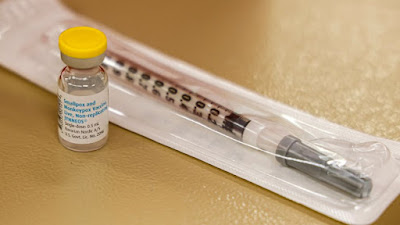 |
| Photo Source: ABC News / AP Photo / Neil Redmond, File |
The ongoing research continues to support the observation that Monkeypox is being spread among MSM through social/sexual networks. Therefore, Monkeypox vaccination as prevention coupled with testing and treatment for HIV, Monkeypox and other STI’s remain to be where efforts need to be focused. The CDC reports that recent findings could lead to expanded Monkeypox vaccination recommendations. The findings may lead to vaccines being recommended for “people with recent STD infections, people with HIV, people taking pre-exposure prophylaxis (PrEP) medications to prevent HIV infection and, possibly, prostitutes”.[5]
Continuing studies will eventually confirm whether HIV infection definitively causes worse outcomes with those infected with monkeypox and/or if simultaneous HIV/STI infection clinically makes someone more susceptible to contracting Monkeypox. However, it is simultaneously important to work towards stopping the spread of the disease.
[1] Simobns, Ranier. (2022, September 1). HIV & Monkeypox: What Patients Need to Know. The ADAP Blog. Retrieved from https://adapadvocacyassociation.blogspot.com/2022/09/hiv-monkeypox-what-patients-need-to-know.html
[2] Hoffman, C. et al. (2022). Clinical characteristics of monkeypox virus infections among men with and without HIV: A large outbreak cohort in Germany. HIV Medicine. Retrieved from https://onlinelibrary.wiley.com/doi/10.1111/hiv.13378
[3] Tarin-Vincente, E., Alemany, A., et al. (2022). Clinical presentation and virological assessment of confirmed human monkeypox virus cases in Spain: a prospective observational cohort study. The Lancet. 400(10353), 661-669. DOI:https://doi.org/10.1016/S0140-6736(22)01436-2
[4] Hein, I. (2022, September 2022). People with HIV more likely to be hospitalized with Monkeypox? Retrieved from https://www.medpagetoday.com/infectiousdisease/hivaids/100628
[5] Stobbe, M. (2022, September 8). US may expand monkeypox vaccine eligibility to men with HIV. Retrieved from https://abcnews.go.com/Health/wireStory/us-expand-monkeypox-vaccine-eligibility-men-hiv-89545619
Disclaimer: Guest blogs do not necessarily reflect the views of the ADAP Advocacy Association, but rather they provide a neutral platform whereby the author serves to promote open, honest discussion about public health-related issues and updates.

No comments:
Post a Comment